For two years, I felt like something was wrong with me — and I couldn’t figure out what. I was tired all the time, even after a full night’s sleep. I felt foggy and unfocused by early afternoon. And my stomach was a constant source of low-level misery: bloating after almost every meal, irregular digestion, that heavy, uncomfortable feeling I’d started to think was just… normal. My “normal.”
I saw a doctor who ran the standard tests and found nothing alarming. I tried cutting gluten, then dairy, then both. Some things helped a little, but the problem never really went away. It wasn’t until I started reading about gut health — really reading, beyond the trendy surface-level content — that I started to understand what might actually be happening. And when I finally addressed my gut health systematically, everything started to shift. The bloating went away. The brain fog lifted. My energy came back. It felt almost too simple to be real.
Today I want to share what I actually did — the specific daily habits that changed my gut health, and why they worked. This isn’t about any single supplement or some 30-day cleanse. It’s about understanding your gut and making small, consistent changes that add up to a genuinely different baseline.
Understanding the Gut-Everything Connection
The gut is often called the “second brain,” and for good reason. Your gut contains its own nervous system — the enteric nervous system — with over 100 million neurons that communicate constantly with your brain via the gut-brain axis. The state of your gut affects your mood, your energy, your immune function, your skin clarity, and your cognitive performance. Everything.
Roughly 70% of your immune system lives in your gut. Most of your serotonin — the “feel good” neurotransmitter — is produced in your gut, not your brain. When your gut microbiome (the community of trillions of bacteria, fungi, and other microorganisms living in your digestive tract) is out of balance, the ripple effects show up everywhere. Fatigue. Brain fog. Skin breakouts. Anxiety. Poor sleep. Constant bloating. In my case, all of the above.
The good news is that the gut microbiome is remarkably responsive to lifestyle changes. Unlike changing your genetics or fixing structural health problems, shifting your gut health is absolutely something you can do through consistent daily habits. Here’s what worked for me.

Habit #1: I Started Taking a Daily Probiotic
This was my first and most impactful change. A quality probiotic introduces beneficial bacteria into your gut and helps restore and maintain a healthy microbiome balance. Not all probiotics are equal, though — I learned this the hard way after spending months on a cheap, low-CFU probiotic that did essentially nothing.
What actually matters when choosing a probiotic:
- CFU count — 10 billion CFU minimum; I personally use 50 billion CFU
- Strain diversity — multiple strains target different aspects of gut health
- Delivery mechanism — the bacteria need to survive stomach acid to reach your gut
- Clinically studied strains — not all probiotic strains have research behind them
- Women-specific formulation — some probiotics are specifically formulated for female microbiome support
I take my probiotic every morning with breakfast, at the same time as my collagen. Consistency matters enormously with probiotics — the benefits build over weeks and months of daily use.

Physician’s CHOICE Probiotics for Women — 50 Billion CFU
Formulated specifically for women’s gut and vaginal health with 6 evidence-backed probiotic strains plus a prebiotic blend. One of the most well-reviewed probiotics on Amazon with over 100K ratings — and for good reason.
Habit #2: I Prioritized Fiber — From Real Food
Fiber is the food your gut bacteria eat. Without adequate fiber, your gut microbiome literally can’t thrive — beneficial bacteria need fermentable fiber (called prebiotics) to survive and multiply. Most Americans consume only about 15 grams of fiber per day, when the recommended amount is 25–38 grams.
I didn’t take a fiber supplement — I added real fiber-rich foods to my meals. Every single day, I now include:
- Vegetables: at least two cups of vegetables at lunch and dinner
- Legumes: lentils, chickpeas, black beans — these are fiber and prebiotic powerhouses
- Whole grains: oats, brown rice, quinoa instead of refined carbs
- Fruit: especially berries, apples (with skin), and pears
- Seeds: chia seeds and flaxseeds sprinkled into smoothies or yogurt
Within two weeks of consistently hitting my fiber goals, my digestion improved more than it had from any supplement or dietary restriction I’d tried before. The bloating that had been my constant companion started to ease up. I wasn’t eliminating anything from my diet — I was adding things in.
Habit #3: I Added Fermented Foods
Fermented foods are naturally rich in probiotics — live, beneficial bacteria that directly contribute to a healthy gut microbiome. Before I started focusing on gut health, I ate essentially zero fermented foods. Now I try to include at least one serving every day.
The fermented foods I rotate through include:
- Plain Greek yogurt — with live active cultures, not the sugary flavored kinds
- Kefir — a fermented dairy drink with a much higher probiotic content than yogurt
- Kimchi — I add this to eggs, rice bowls, and grain salads
- Sauerkraut — the refrigerated kind, not the shelf-stable pasteurized version
- Kombucha — I drink this a few times a week as a soda alternative
The key is variety — different fermented foods contain different bacterial strains, so rotating through them builds a more diverse microbiome.

Garden of Life Dr. Formulated Probiotics for Women 50 Billion CFU
Formulated by David Perlmutter, MD, this probiotic includes 16 targeted strains plus prebiotics and supports digestive health, vaginal health, and immune function. Non-GMO, raw, and shelf-stable.

Habit #4: I Got Serious About Hydration
This sounds almost embarrassingly simple, but staying properly hydrated is one of the most underrated things you can do for gut health. Water helps move fiber through your digestive system and prevents constipation. When you’re dehydrated, everything slows down — and a sluggish digestive system is a breeding ground for bloating, discomfort, and the kind of off feeling that’s hard to name but easy to live with unfortunately.
I started tracking my water intake and aimed for about 80–100 ounces per day (I run hot and exercise regularly, so I need more than the standard eight glasses). I noticed a difference in my digestion within days. It wasn’t dramatic, but the baseline discomfort I’d had for so long just… quieted down.
Habit #5: I Reduced Ultra-Processed Foods
I want to be clear: I did not go on any kind of strict diet. I didn’t eliminate any food group or make any dramatic cutbacks. But I did start paying attention to how I felt after eating ultra-processed foods — things like chips, packaged snack foods, fast food, and foods with long lists of artificial ingredients — and the correlation was undeniable. Every time I had a big serving of ultra-processed food, I’d feel bloated and sluggish within a couple of hours.
The reason is that many ultra-processed foods contain emulsifiers, artificial sweeteners, and other additives that can disrupt the gut microbiome and increase intestinal permeability. I didn’t need to cut them out completely — I just started making them the exception rather than the norm. Swapping a bag of chips for a handful of nuts and an apple several times a week made a measurable difference.
Habit #6: I Addressed My Stress (For Real This Time)
The gut-brain axis works both ways. Stress doesn’t just feel bad — it physiologically changes your gut environment. Chronic stress elevates cortisol, which disrupts the gut microbiome, increases inflammation in the gut lining, and slows or disrupts digestion. The phrase “nervous stomach” exists because the connection between anxiety and gut symptoms is very, very real.
I started a simple daily breathwork practice — five minutes in the morning, ten minutes before bed. Box breathing or simple diaphragmatic breathing activates the parasympathetic nervous system (the “rest and digest” mode), which directly supports better gut function. I also started a journaling habit to process the mental load I’d been carrying around. Both of these felt frivolous at first. Neither of them was.
Habit #7: I Prioritized Sleep
This one took me longest to take seriously. Poor sleep disrupts the gut microbiome — studies have shown that even one night of poor sleep can negatively impact gut bacterial diversity. Conversely, a healthy gut produces neurotransmitters and hormones that support better sleep. The relationship between sleep and gut health is circular: fix one, and the other improves.
I started protecting my sleep window more aggressively: a consistent bedtime and wake time (even on weekends), no screens in the hour before bed, and a cooler bedroom temperature. My sleep improved, my gut improved, and my overall energy went from “dragging” to something I might dare call “good.”
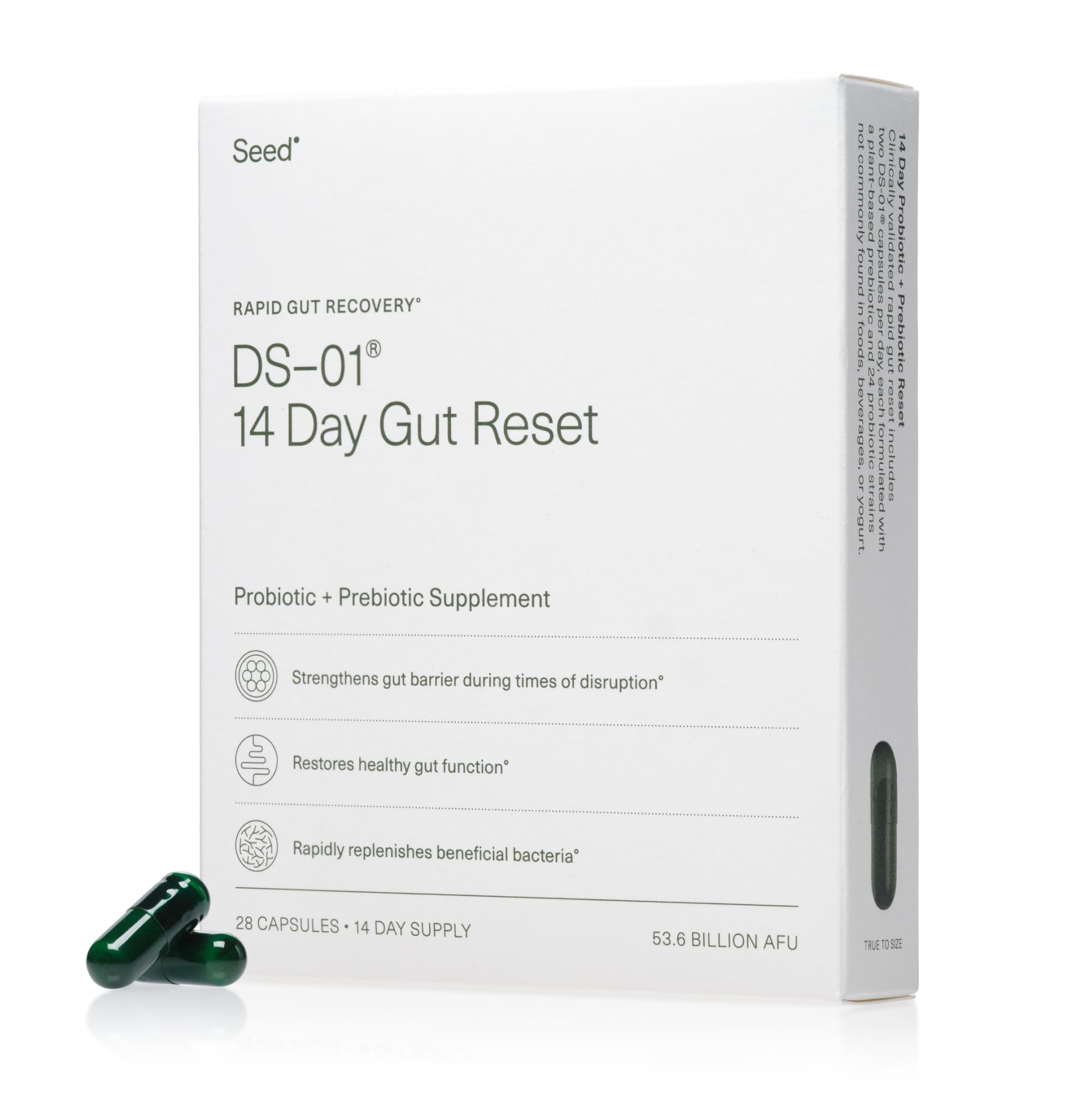
Seed DS-01 Daily Synbiotic — Probiotic + Prebiotic for Women
The most advanced probiotic on the market — a 2-in-1 synbiotic (probiotic + prebiotic) with 24 clinically studied strains. Seed’s patented delivery technology ensures the bacteria actually survive to reach your gut.
What My Gut Health Routine Looks Like Now
Eight months into these habits, my gut feels completely different. The bloating that used to be my constant companion is essentially gone. My digestion is regular and comfortable. The brain fog I’d written off as just part of being a busy adult has lifted to the point where I feel noticeably sharper and more focused in the afternoons. My skin is clearer. My mood is more stable. I have actual energy.
None of this happened overnight. But it also didn’t require anything drastic. The changes were small, consistent, and layered over time. That’s what gut health is — it’s not a reset or a cleanse. It’s a long-term practice of supporting the trillions of organisms that make your body work.
If you’re struggling with bloating, brain fog, fatigue, or any of the symptoms I described, please know: this is not just your normal. Your gut can get better. Start with one habit from this list and build from there. The changes will compound in ways you don’t expect.
Foods That Harm Your Gut Health
We spend a lot of time talking about what to eat for gut health — but knowing what to limit is just as important. I’m not about strict elimination or food fear, but I did find that cutting back on certain things made a noticeable difference in how my gut functioned, even when everything else stayed the same. Here’s what the research — and my own experience — points to.
Ultra-Processed Foods
I touched on this in the habits section, but it bears repeating: ultra-processed foods are consistently linked to reduced gut microbiome diversity, increased intestinal permeability (leaky gut), and elevated inflammation. The issue isn’t just what they contain — it’s what they lack. Ultra-processed foods are stripped of the fiber and polyphenols that gut bacteria need to thrive, and they often contain additives like emulsifiers and artificial sweeteners that may disrupt the gut lining. If there’s one thing to minimize, this is it.
Artificial Sweeteners
This one surprised me when I first learned about it. Research suggests that certain artificial sweeteners — particularly saccharin, sucralose, and aspartame — may negatively alter gut microbiome composition and impair glucose metabolism, even without actual sugar. I swapped my diet soda habit for sparkling water with a squeeze of lemon and noticed a real difference in my bloating levels within a few weeks. If you’re using a lot of zero-calorie sweeteners, it may be worth experimenting with reducing them.
Excessive Alcohol
Alcohol is genuinely tough on the gut. It can damage the gut lining, promote the growth of harmful bacteria, and reduce the diversity of beneficial strains. Even moderate drinking can affect gut permeability. I’m not saying never drink — I still enjoy a glass of wine on weekends — but if you’re actively trying to heal your gut, giving alcohol a break (even for a few weeks) can make a significant difference in how you feel.
High-Sugar Foods and Refined Carbohydrates
Sugar feeds the wrong kinds of bacteria in your gut — specifically the types associated with inflammation and dysbiosis (an imbalance of gut microbes). Refined carbohydrates like white bread, pastries, and sugary cereals spike blood sugar and break down quickly with little fiber benefit. This doesn’t mean you can never eat these things, but if bloating, gas, or digestive discomfort are regular issues for you, temporarily reducing refined sugar and processed carbs is one of the most effective dietary interventions you can make.
Fried and High-Fat Processed Foods
Greasy, heavily fried foods can slow gut motility (the speed at which food moves through your digestive system), promote inflammation, and displace the fiber-rich foods your gut microbiome actually needs. Occasional fries aren’t going to derail you, but a diet heavy in fried food tends to correlate with reduced microbiome diversity. If fast food is a regular habit, replacing even a few of those meals weekly with whole-food alternatives will likely make a noticeable difference.
Frequently Asked Questions About Gut Health
How long does it take to improve gut health?
The encouraging answer is that your gut microbiome can start responding to dietary changes relatively quickly — some studies show measurable shifts in microbiome composition within 3–5 days of changing your diet. However, meaningful, lasting improvement in symptoms like bloating, digestion, and energy typically takes 4–8 weeks of consistent habits. Full restoration after a period of poor gut health or antibiotic use may take several months. The key is consistency: your gut rewards you for showing up every day with fiber, fermented foods, hydration, and stress management.
What are the signs of an unhealthy gut?
The symptoms of poor gut health are more wide-ranging than most people realize. Beyond the obvious digestive issues — bloating, gas, constipation, diarrhea, or irregular bowel movements — an unhealthy gut can manifest as persistent fatigue, brain fog, skin issues like acne or eczema, frequent colds (due to compromised immune function), mood swings, food intolerances, and even anxiety or depression. The gut-brain axis means your gut health has a direct line to your mental and emotional state, which is why improving your gut can feel like a full-body and full-mind transformation.
Are probiotic supplements worth it?
The evidence for probiotic supplements is genuinely promising, particularly for specific strains and specific conditions. For general gut health maintenance, a high-quality multi-strain probiotic with clinically studied strains (look for Lactobacillus and Bifidobacterium species with published research) can be a worthwhile addition to your routine. That said, probiotics are most effective when paired with a fiber-rich diet — the fiber is what the good bacteria eat and thrive on. A probiotic without dietary fiber is like planting seeds in soil with no nutrients. Do both.
Can stress really cause gut problems?
Absolutely — and this is one of the most underappreciated aspects of gut health. The gut and brain are in constant two-way communication via the vagus nerve (part of the gut-brain axis). When you’re stressed, your body activates the “fight or flight” response, diverting blood flow away from digestion and toward your muscles and heart. Chronic stress alters gut motility, increases intestinal permeability, reduces beneficial bacteria populations, and can trigger or worsen conditions like IBS. Managing stress isn’t just mental health advice — it’s a genuine gut health intervention.
Is it possible to heal leaky gut?
Leaky gut (intestinal permeability) refers to a condition where the tight junctions of the gut lining become compromised, allowing substances to pass through the gut wall that shouldn’t. While it’s still an evolving area of research, there is good evidence that dietary and lifestyle changes can meaningfully improve gut barrier function. Key strategies include removing gut irritants (processed foods, alcohol, NSAIDs), adding gut-supportive foods (bone broth, fermented foods, zinc-rich foods), managing stress, and optimizing sleep. Many people report significant improvement in symptoms over a period of months with consistent effort.
Do I need to do a gut cleanse or reset?
I’ll be honest with you: most commercial gut cleanses and detox programs are not supported by strong scientific evidence, and some can actually disrupt your microbiome further. Your gut doesn’t need a dramatic reset — it needs consistent daily support. The habits I’ve described in this post (fiber, fermented foods, hydration, stress management, sleep, reduced ultra-processed foods) are far more effective than any short-term cleanse. If you feel like you need a “reset,” treat it as a signal to get back to the fundamentals rather than reach for a laxative tea or juice fast.
Free Download
Get My Daily Supplement Stack Guide
Everything I take, why I take it, and what I noticed — morning, midday, and evening. Free when you join the list.
No spam, ever. Unsubscribe anytime.



